If you are planning to get pregnant or want to proactively manage your reproductive health, AMH level is a key indicator you must understand. In the field of reproductive medicine, AMH is widely recognized as the most stable and convenient biomarker for assessing women’s ovarian reserve. It is not affected by the menstrual cycle, oral contraceptives, or pregnancy, and can be tested at any time.
What is AMH Level?
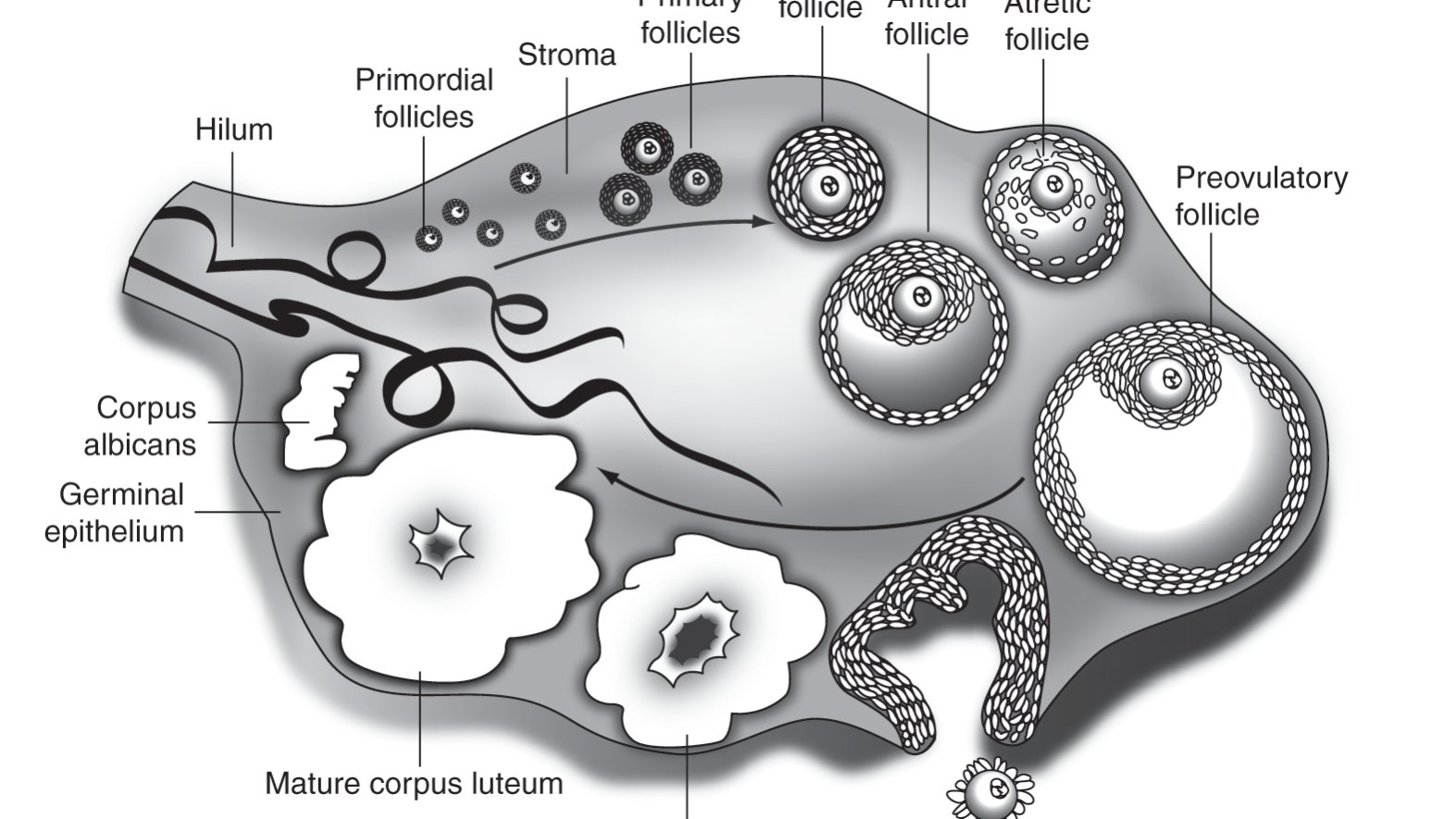
AMH (Anti-Müllerian Hormone) is secreted by the granulosa cells of small antral follicles in the ovaries and directly reflects the quantity of remaining “egg inventory” in the ovaries. Higher values (within the normal range) generally indicate better ovarian reserve; lower values suggest fewer eggs in reserve. The core physiological role of AMH is to inhibit the premature activation of primordial follicles, slowing the rate of follicle depletion and thereby “protecting” the ovarian reserve. This characteristic makes AMH the preferred indicator for evaluating ovarian function.
Four Major Clinical Applications of AMH Level
1. Assessing Ovarian Reserve Function
AMH can accurately reflect “ovarian age”, detecting a decline in reserve earlier than traditional FSH testing (up to 5–10 years earlier). The WHO infertility guidelines clearly state that when performing ovarian reserve testing, priority can be given to AMH, antral follicle count (AFC), or FSH on days 2–3 of the menstrual cycle.
2. Guiding IVF (In Vitro Fertilization) Protocols
AMH is a key basis for doctors in formulating ovarian stimulation protocols: AMH ≤1.1 ng/mL suggests a potentially poor ovarian response, requiring adjustment of medication dosage to improve success rates. The ESHRE “Bologna criteria” list abnormal ovarian reserve testing (such as low AMH) as one of the core criteria for defining poor ovarian response.
3. Assisting in the Diagnosis of Polycystic Ovary Syndrome (PCOS)
4. Predicting the Timing of Menopause
AMH naturally declines with age. Multiple studies confirm that when AMH <0.2 ng/mL, the average remaining time to menopause is approximately 5–10 years, a conclusion widely cited in international reproductive medicine guidelines.
Age-Specific Reference Ranges for AMH Level
The following data are based on a large cohort study of 22,920 women of reproductive age published by PMC (U.S. National Institutes of Health), serving as internationally accepted age-stratified reference ranges:
- 20–30 years: 2.0–7.0 ng/mL
- 31–35 years: 1.5–6.0 ng/mL
- 36–40 years: 0.8–4.0 ng/mL
- Above 40 years: usually <1.0 ng/mL, with most <0.8 ng/mL
Important Note: AMH only reflects egg quantity and is not directly equivalent to egg quality. Age is the core factor affecting egg quality; young women with low AMH may still have high-quality eggs.
Can Declining AMH Be Reversed?
Age-related decline: Irreversible; currently, no medical means can “turn back the clock.”
Non-age-related factors (stress, obesity, disease, medications, etc.): After removing the triggers, AMH may partially recover. For example, obese women who lose 5%–10% of body weight can see significant improvement in AMH levels.
Scientific interventions can slow the decline (international reproductive medicine consensus):
- Regular sleep schedule, avoid staying up late (sleep deprivation accelerates follicle depletion)
- Balanced diet, increase intake of antioxidants (vitamin C, E) and high-quality protein
- Moderate exercise, maintain a healthy weight (BMI 18.5–24.9)
- Quit smoking and limit alcohol; smoking lowers AMH and advances menopause by 1–2 years
- Manage stress to reduce cortisol’s inhibitory effect on the ovaries
Who Should Test AMH?
- Women over 30 with fertility plans (ovarian reserve declines significantly after age 30)
- Those with irregular menstruation or infrequent ovulation (suspected ovulatory dysfunction or PCOS)
- Women preparing for IVF or other assisted reproduction (to guide protocol design)
- Suspected PCOS cases (combine symptoms with AMH for auxiliary diagnosis)
- Those who have undergone ovarian surgery, chemotherapy, or radiotherapy (to assess damage to ovarian reserve)
- Those with a family history of premature menopause or primary ovarian insufficiency (POI)
- Women with unexplained infertility (to rule out ovarian reserve issues)
- Women under 40 with menstrual abnormalities lasting more than 4 months (to screen for POI)
AMH and Common Reproductive Disorders (Authoritative Diagnostic Criteria)
1. Primary Ovarian Insufficiency (POI)
Diagnostic criteria:
② Oligomenorrhea or amenorrhea ≥4 months;
③ FSH >25 IU/L (re-test after 4–6 weeks);
④ AMH <1.0 ng/mL (auxiliary confirmation, especially useful when FSH results are uncertain).
Fertility in POI patients is significantly reduced; early intervention is needed to slow ovarian function decline.
2. Polycystic Ovary Syndrome (PCOS)
Core association: AMH levels are usually 2–3 times higher than in healthy women. AMH cannot be used alone to diagnose PCOS; diagnosis requires at least two of the following: ovulatory dysfunction, hyperandrogenism, and polycystic ovarian morphology (or high AMH), while excluding other causes.
3. Age-Related Ovarian Decline
After age 35, AMH enters a rapid decline phase, with significantly reduced natural conception rates and embryo euploidy rates. WHO guidelines emphasize that age is the core predictor of ovarian reserve, and AMH testing can serve as a supplement to age assessment, helping women plan fertility earlier.
Conclusion
AMH is a “window” into understanding ovarian reserve, providing objective evidence for fertility planning and health management. Regular monitoring of AMH, combined with scientific interventions, is key to proactively managing reproductive health. Regardless of whether the value is high or low, understanding AMH is the first step toward taking control of your reproductive future.
Please note that AMH test results can vary depending on the testing platform; interpretation should refer to the reference range provided by the testing institution, and cross-platform comparisons should be avoided.
Find out more about fertility and female health from ENERBABY.